Methamphetamine abuse is a huge problem within the United States, and because of its potency, the drug can lead to rapid dependency. By the time many users realize they have a problem and try to quit, they find that the withdrawal effects have become too powerful to overcome on their own. Undergoing withdrawal in a medical detox program is the safest way to treat symptoms and remove meth from the body, before committing to full recovery. These programs support patients with around-the-clock medical care throughout the entire process. Doctors and nurses are able to monitor patients’ vitals and tailor treatment plans as withdrawal symptoms begin to improve. Once detox is complete, recovering users can seek counseling and other services to learn how to maintain long-term sobriety.
Meth Withdrawal Symptoms
Symptoms of meth withdrawal may include:
- Feelings of fatigue, lethargy, and excessive sleepiness (typical of withdrawal from stimulant medications) are common.
- Increased appetite, dry mouth, and some episodes of jitteriness generally occur.
- Depression, apathy, feelings of hopelessness, and thoughts of suicide.
- Extreme cravings for more meth.
- Psychotic symptoms such as paranoia, hallucinations, and delusions.
A significant number of individuals report feelings of depression, which were also noted to decline in a linear fashion over the course of the withdrawal time period. These depressive symptoms can be significant and associated with thoughts of suicide. In addition, research has indicated that a good number of individuals who relapse do so because of feelings of depression, apathy, hopelessness, etc.
Jump To Section
Meth Comedown: Feelings Of Hopelessness
Meth’s effects may last for up to eight hours, depending on the dose, but once the drug starts to wear off, the comedown effects can cause the individual to feel terrible.
A comedown is different from withdrawal, although there are a few aspects of the process that appear similar. Comedowns from drugs are closer to hangovers from alcohol, as both are caused by a combination of neurotransmitter imbalances in the brain, chemicals metabolized into toxins that build up in the body, and exhaustion from the euphoria of the drug.
Meth comedown symptoms include:
- Hopelessness
- Sadness
- Depression
- Muscle weakness
- Decreased appetite
- Fatigue
- Lack of motivation
- Anxiety
- Insomnia despite exhaustion
- Headache from dehydration
- Muscle pain, especially in the jaw from clenching
Comedown symptoms may last for a few days after one abuses the drug, especially mental health changes like depression and anxiety. When abused as a party drug, meth may be mixed with other amphetamines, opioids, or alcohol. Mixing drugs together is very dangerous and can cause an overdose; in addition, comedown symptoms will feel worse or more intense when substances are combined. If the individual does not take any more meth, these symptoms will resolve on their own.
Meth Withdrawal Timeline
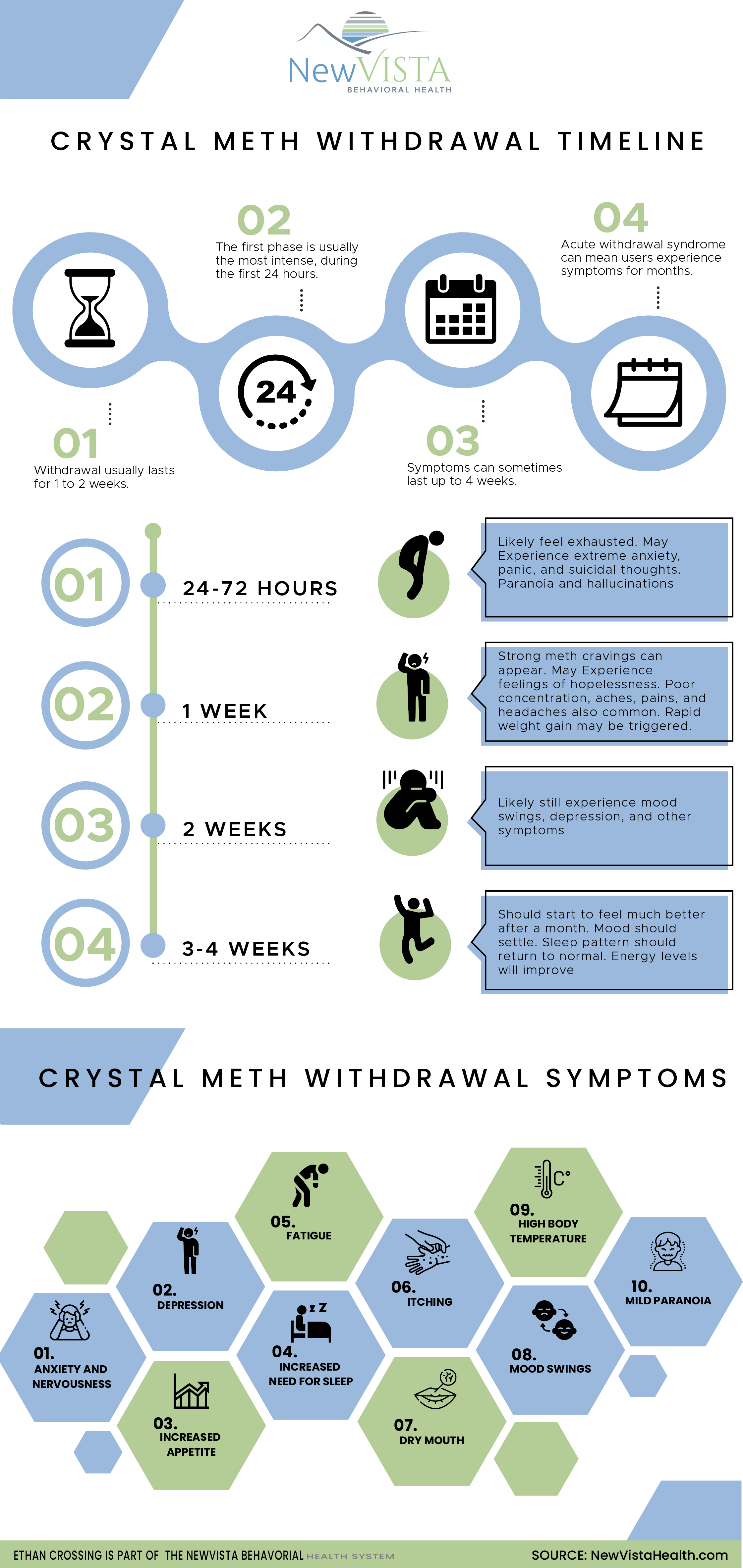
The specific time period for withdrawal varies between individuals, but the acute phase of withdrawal typically peaks around day 2 or 3 after last use and generally begins to ease after a week. However, psychological symptoms including mood swings, agitation, drug cravings, and sleep disturbances can persist for multiple weeks and depression can last for even months to a year in some.
| Duration of Meth Withdrawals: Timeline of Symptoms | |
| First 48 Hours | This phase is known as the “crash” and occurs within the first day of stopping the use of the drug. During the first 24-48 hours, former users will begin to experience a sharp decline in energy and cognitive function, as well as nausea, abdominal cramping, and sweating. |
| Days 3-10 | Withdrawal symptoms typically peak during this time. As the body attempts to adjust without Meth, recovering users will experience severe depression, anxiety, and extreme fatigue. Some people will also experience shaking and lingering muscle aches, as well as intense drug cravings. |
| Days 14-20 | Symptoms of Meth withdrawal typically last around 2-3 weeks. Towards the end of the second week, most physical symptoms begin to subside, but intense drug cravings can persist. Additionally, continuing fatigue and depression are common during this period. |
| 1 Month+ | The worst withdrawal symptoms are typically over at this point. Any remaining symptoms will continue to fade over time. However, for some, the psychological symptoms such as depression and anxiety may continue for several months before they subside. |
How Detox Can Help Long-Term Meth Recovery
Many individuals may feel hesitant to begin a detox, but rest assured that the top priority of any detox center is for patients to feel safe and comfortable during the process when attending treatment. The detox process is broken down into 3 stages to ensure patients receive the form of care that’s right for them.
Evaluation
Upon admission, a medical team will assess the patient’s health and well-being. Doctors and nurses typically use urine drug screens to determine the amount of meth that a patient has used recently. From there, the treatment team can develop a detox plan that fits their specific needs. Keep in mind that the doctor may ask a patient questions about their current and past substance abuse. This is necessary for setting up a patient’s long-term recovery plan. It’s also helpful for doctors to know if the patient suffers from any co-occurring disorders, as these can affect the types of detox treatments the patient will receive.
Stabilization
Many patients who arrive at the detox center are experiencing the peak of their withdrawal symptoms. Treatments begin as soon as possible after the evaluation stage to help make the patient more comfortable. As symptoms improve, doctors will adjust treatments accordingly. Medical staff will also keep the patient’s loved ones informed and updated on their progress.
Transition Into Further Treatment
When the detox process is almost complete, doctors will begin to discuss the next steps with their patients. Detox is only the first step in meth addiction treatment, and physicians recommend that patients continue their recovery in a rehab facility. If the detox is already taking place in a treatment facility, medical staff will help patients transition into the next stage and stay on track toward sobriety.
Medications Used To Assist Meth Withdrawal
There are several different medications that can help to manage some of the symptoms that occur during this process of withdrawal:
- Wellbutrin (bupropion): This drug is an antidepressant that has been approved for and used in smoking cessation programs. It also has a good body of research indicating that it is useful in reducing the symptoms of withdrawal in individuals who have abused crystal meth. It appears to reduce the significant cravings associated with the withdrawal process and appears to be more appropriate for light to moderate methamphetamine use disorders.
- Provigil (modafinil): This medication is a mild stimulant medication that is used in the treatment of ADHD and in the treatment of narcolepsy. The mild stimulant properties of the medication can assist in reducing issues with disruptive sleep patterns and may also help those in recovery with increasing energy and enhancing concentration.
- Selective serotonin reuptake inhibitors: Paxil (paroxetine) is a selective serotonin reuptake inhibitor (a specific type of antidepressant medication) that has been shown in some studies to relieve cravings in abstinent crystal meth users going through withdrawal; however, the research on the efficiency of this drug for treatment during crystal meth withdrawal is mixed. There is research that has suggested that Prozac (fluoxetine) may be useful in the treatment of crystal meth addiction during the withdrawal process.
- Remeron (mirtazapine): Remeron is an atypical antidepressant that has its primary mechanism of action on both serotonin and norepinephrine. There is evidence that its use can help to prevent relapse during the withdrawal process.
In the management of the withdrawal process from meth, physicians are free to use any medications to address any specific symptoms that occur in individuals. For instance, in individuals who develop psychotic-type behaviors, such as paranoia, delusions, and/or hallucinations, physicians are free to administer antipsychotic medications to these individuals if the symptoms are judged to be severe enough to require direct treatment.